Patients
Cirrhosis of the Liver
The liver weighs about three pounds and is the largest organ in the body. It is located in the upper right side of the abdomen, below the ribs. When chronic diseases cause the liver to become permanently injured and scarred, the condition is called cirrhosis.The scar tissue that forms in cirrhosis harms the structure of the liver, blocking the flow of blood through the organ. The loss of normal liver tissue slows the processing of nutrients, hormones, drugs, and toxins by the liver. Also slowed is production of proteins and other substances made by the liver.
What is the Impact of Cirrhosis?
Cirrhosis is the eleventh leading cause of death by disease in the United States. Almost one-half of these are alcohol related. About 25,000 people die from cirrhosis each year. There also is a great toll in terms of human suffering, hospital costs, and the loss of work by people with cirrhosis.
What are the Major Causes of Cirrhosis?
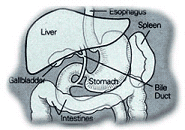 Cirrhosis
has many causes. It can result from direct injury to the liver cells (i.e.,
hepatitis) or from indirect injury via inflammation or obstruction to bile ducts
which drain the liver cells of bile. Common causes of direct liver injury
include chronic alcoholism (most common cause in the United States), chronic
viral hepatitis (types B, C, and D) and auto immune hepatitis. Common causes of
indirect injury by way of bile duct damage include primary biliary cirrhosis,
primary sclerosing cholangitis and biliary atresia (common cause of cirrhosis in
infants).
Cirrhosis
has many causes. It can result from direct injury to the liver cells (i.e.,
hepatitis) or from indirect injury via inflammation or obstruction to bile ducts
which drain the liver cells of bile. Common causes of direct liver injury
include chronic alcoholism (most common cause in the United States), chronic
viral hepatitis (types B, C, and D) and auto immune hepatitis. Common causes of
indirect injury by way of bile duct damage include primary biliary cirrhosis,
primary sclerosing cholangitis and biliary atresia (common cause of cirrhosis in
infants).Less common causes of cirrhosis include direct liver injury from inherited disease such as cystic fibrosis, alpha-1-antitrypsin deficiency, hemochromatosis, Wilson's disease, galactosemia, and glycogen storage disease.
Two inherited disorders result in the abnormal storage of metals in the liver leading to tissue damage and cirrhosis. People with Wilson's disease store too much copper in their liver, brain, kidneys, and in the corneas of their eyes.
In another disorder, known as hemochromatosis, too much iron is absorbed, and the excess iron is deposited in the liver and in other organs, such as the pancreas, skin, intestinal lining, heart and endocrine glands.
If a person's bile duct becomes blocked, this also may cause cirrhosis. The bile ducts carry bile formed in the liver to the intestines, where the bile helps in the digestion of fat.
In babies, the most common cause of cirrhosis due to blocked bile ducts is a disease called biliary atresia. In this case, the bile ducts are absent or injured, causing the bile to back up in the liver. These babies are jaundiced (their skin is yellowed) after their first month of life. Sometimes they can be helped by surgery in which a new duct is formed to allow bile to drain again from the liver.
In adults, the bile ducts may become inflamed, blocked, and scarred due to another liver disease, primary biliary cirrhosis. Another type of biliary cirrhosis also may occur after a patient has gallbladder surgery in which the bile ducts are injured or tied off.
Very rare causes of cirrhosis include: reactions to drugs (e.g., vitamin A, methotrexate, amiodarone) exposure to environmental toxins, and repeated bouts of heart failure with liver congestion.
f after full evaluation of a patient with cirrhosis, the etiology still is not clear, the disease is called "cystogenic cirrhosis." As much as 10 percent of cirrhosis falls into this category.
What are the Symptoms of Cirrhosis?
 People
with cirrhosis often have few symptoms at first. The two major problems that
eventually cause symptoms are loss of functioning liver cells and distortion of
the liver caused by scarring. The person may experience fatigue, weakness, and
exhaustion. Loss of appetite is usual, often with nausea and weight loss. Some
patients present with menstrual abnormalities (amenorrhea), impotence, loss of
sexual drive or painfully enlarged breasts (in men).
People
with cirrhosis often have few symptoms at first. The two major problems that
eventually cause symptoms are loss of functioning liver cells and distortion of
the liver caused by scarring. The person may experience fatigue, weakness, and
exhaustion. Loss of appetite is usual, often with nausea and weight loss. Some
patients present with menstrual abnormalities (amenorrhea), impotence, loss of
sexual drive or painfully enlarged breasts (in men).As liver function declines, less protein is made by the organ. For example, less of the protein albumin is made, which results in water accumulating in the legs (edema) or abdomen (ascites). A decrease in proteins needed for blood clotting makes it easy for the person to bruise or to bleed.
In the later stages of cirrhosis, jaundice (yellow skin) may occur, caused by the buildup of bile pigment that is normally passed by the liver into the intestines. Some people with cirrhosis experience intense itching due to bile products that are deposited in the skin. Gallstones often form in persons with cirrhosis because not enough bile reaches the gallbladder.
The liver of a person with cirrhosis also has trouble removing toxins, which may build up in the blood. These toxins can dull mental function and lead to personality changes and even coma (encephalopathy). Early signs of toxin accumulation in the brain may include neglect of personal appearance, unresponsiveness, forgetfulness, trouble concentrating, or changes in sleeping habits.
Drugs taken usually are filtered out by the liver, and this cleansing process is also slowed down by cirrhosis. The liver does not remove the drugs from the blood at the usual rate, so the drugs act longer than expected, building up in the body. People with cirrhosis are often very sensitive to medications and their side effects.
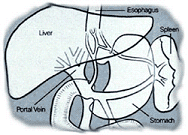
A serious problem for people with cirrhosis is pressure on blood vessels that flow through the liver. Normally, blood from the intestines and spleen is pumped to the liver through the portal vein. But in cirrhosis, this normal flow of blood is slowed, building pressure in the portal vein (portal hypertension). This blocks the normal flow of blood, causing the spleen to enlarge. So blood from the intestines tries to find a way around the liver through new vessels.
Some of these new blood vessels become quite large and are called "varices." These vessels may form in the stomach and esophagus (the tube that connects the mouth with the stomach). They have thin walls and carry high pressure. There is great danger that they may break, causing a serious bleeding problem in the upper stomach or esophagus. If this happens, the patientÕs life is in danger, and the doctor must act quickly to stop the bleeding.
How is Cirrhosis Diagnosed?
The doctor often can diagnose cirrhosis from the patient's symptoms and from laboratory tests. During a physical exam, for instance, the doctor could notice a change in how your liver feels or how large it is. If the doctor suspects cirrhosis, you will be given blood tests. The purpose of these tests is to find out if liver disease is present. In some cases, other tests that take pictures of the liver are performed such as the computerized axial tomography (CAT) scan, ultrasound, and the radioisotope liver/spleen scan.
The doctor may decide to confirm the diagnosis by putting a needle through the skin (biopsy) to take a sample of tissue from the liver. In some cases, cirrhosis is diagnosed during surgery when the doctor is able to see the entire liver. The liver also can be inspected through a laparoscope, a viewing device that is inserted through a tiny incision in the abdomen.
What are the Treatments for Cirrhosis?
Treatment of cirrhosis is aimed to stop the development of scar tissue in the liver and prevent complications. When cirrhosis is due to an identifiable cause, treatment programs may be specific, such as for management of hepatitis B and C, or steroids and immunosuppressive agents for auto-immune chronic active hepatitis.
No matter what the cause of cirrhosis, every patient must avoid all substances, habits, and drugs that may further damage the liver, precipitate complications, or speed the progression to liver failure. Alcohol, in addition to causing cirrhosis, may accelerate the progression of liver scarring due to other causes, such as hepatitis C. All patients with liver disease should not drink alcoholic beverages. Even some non-prescription drugs and vitamins, acetaminophen, in relatively small doses (more than five doses a day) and Vitamin A (more than 25,000 IU/day) may precipitate liver failure. Non-steroidal anti-inflammatory drugs, such as ibuprofen, may precipitate severe bleeding and/or kidney failure.
The cirrhotic patient is at increased risk of contracting other infections that may be more severe than in healthy patients. Immunizations for hepatitis A, B, influenza, and pneumococcal pneumonia are available and should be administered. Raw seafood may contain bacteria that can cause life-threatening infections and therefore should be avoided.
How are the Complications of Cirrhosis Treated?
The abnormal accumulation of fluid may cause swelling of the ankles (edema) and abdomen (ascites). Therefore, patients should reduce the amount of fluid and salt in their diet or use drugs called "diuretics" that mobilize and excrete the excess fluid through the kidneys. Occasionally, the ascites may become infected, a condition known as Spontaneous Bacterial Peritonitis, and require treatment with antibiotics.
When the liver does not efficiently function to cleanse the body of toxins and drugs, the mental state of patients may change dramatically and lead to coma, called Hepatic Encephalopathy. Treatment is directed at reducing the protein in the diet, avoiding sedatives and pain medications, and using laxatives and/or antibiotics to decrease the absorption of toxins from the intestines.
Sometimes, bleeding from the esophagus or stomach caused by abnormal veins (varices) may occur and is a life-threatening emergency requiring hospitalization. Variceal bleeding can usually be controlled with the use of a flexible tube (endoscope) that is inserted through the mouth into the esophagus and stomach and used to inject clotting agents into the veins or to rubberband ligate the varices.
Liver failure refers to the end stage of liver disease and cirrhosis when the liver stops working and cannot support life. Liver failure is difficult to treat and survival is limited. Therefore, patients with any complication of cirrhosis are considered to be at risk of developing liver failure.
When complications develop, it may be possible to manage them. When it is likely that liver failure will develop, some patients with cirrhosis are able to undergo liver transplantation. The treating gastroenterologist may recommend liver transplantation when complications of cirrhosis develop in an attempt to avoid liver failure.